 An abnormal ECG was recorded in 1 patient in the monotherapy subgroup and in 10 patients in the polytherapy subgroup ( p = 0.05). However, we observed a relationship between ECG changes and the number of AEDs taken. The type of AEDs (including CBZ) did not have a significant influence on the ECG trace. 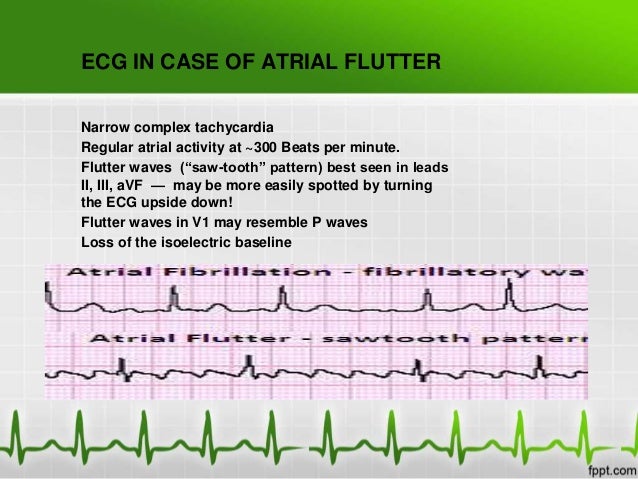
10.71% p = 0.04), which is significant in connection with the reports of a higher risk of SUDEP in males. On the 24-hour ECG changes were more frequent in male than female patients (46.43% vs. The following were present: VEs ( n = 28 56%), SVEs ( n = 23 46%), bradycardia ( n = 13 26%), tachycardia ( n = 9 18%), pairs/triplets ( n = 3 6%), bigeminy ( n = 3 6%), trigeminy ( n = 2 4%), AV block IIº ( n = 2 4%) and pause ( n = 1 2%). In all NTPs with bradycardia (22.7%) paroxysmal EEG changes were recorded.Ĭhanges on the 24-hour ECG were more frequent in NTPs than TPs, which did not confirm the adverse effect of AEDs on ECG as reported by many authors. The following were observed: significant J-point elevation ( n = 9 18%), bradycardia ( n = 5 10%), RBBB ( n = 4 8%), shortening of QTc ( n = 3 6%), QTc prolongation ( n = 1 2%), LGL syndrome ( n = 1 2%), AV block Iº ( n = 1 2%), LBBB ( n = 1 2%) and SVEs ( n = 1 2%). On the resting ECG, changes were recorded in 10 NTPs (45.45%) and 11 TPs (39.29%). Paroxysmal EEG changes were related to a higher number of seizures over the last month and treatment with carbamazepine ( p = 0.05). The analysis showed a significantly higher value of 24-hour EEG for the detection of abnormal seizure activity ( p = 0.02). On the routine EEG, paroxysmal changes were observed in 12 NTPs (54.55%) and 14 TPs (50%) on the 24-hour EEG in 14 NTPs (63.64%) and 19 TPs (67.86%). The following tests were used in the statistical analysis: χ 2, Shapiro- Wilk, Student’s t-test, ANOVA, Mann-Whitney U test and Kruskal-Wallis test. Subjects with cardiovascular disease, accompanying metabolic and/or electrolyte disturbances, alcohol abuse, and those on medications other than AEDs were excluded from the study. Twenty-two non-treated patients (NTPs) with newly diagnosed epilepsy before the inclusion of AEDs (mean age: 36.1 ☑2.1 years) and 28 patients with epilepsy treated with AEDs (TPs) for at least 2 years (mean age: 29.6 ☘.7 years) were enrolled in the study. The aim of our study was to assess the occurrence of changes on EEG and ECG in EPs. Detection of ECG changes is also important because of the phenomenon of sudden unexpected death in epilepsy (SUDEP). ECG changes could also be explained by the influence of epileptic discharges on the central autonomic nervous system, the effect of antiepileptic drugs (AEDs) and the presence of genetically determined disorders of ion channel function. However, an abnormal ECG trace requires the exclusion of heart disease and verification of the diagnosis of epilepsy. 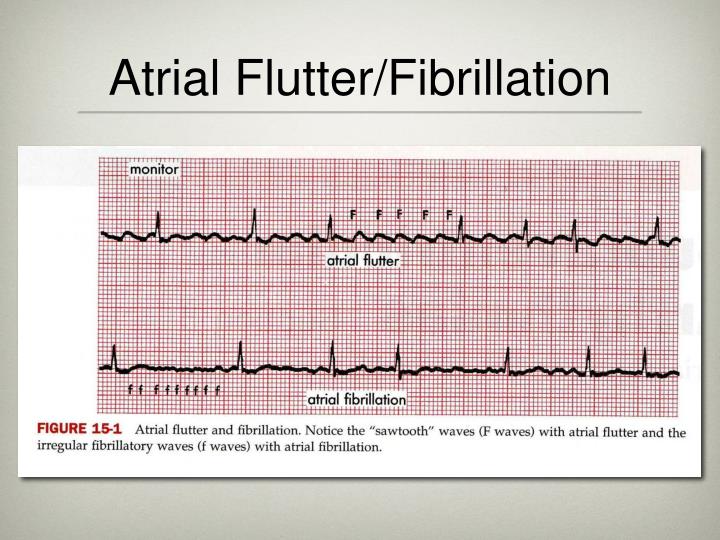
An abnormal EEG is not surprising in EPs. Changes on electroencephalography (EEG) and electrocardiography (ECG) may occur in epileptic patients (EPs) both during epileptic seizures and in the interictal period. 
0 Comments
Leave a Reply. |

 RSS Feed
RSS Feed
